At present, the goal of allergic rhinitis treatment is to control symptoms, as a complete cure is rarely available. However, for people whose symptoms are not adequately managed with standard treatments, allergen immunotherapy may be an option. This is currently the only treatment shown to alter the course of the disease, away from allergy and towards tolerance of the allergen(s) triggering the symptoms.
Your healthcare provider will work with you to review your symptoms and to adjust your treatment plan accordingly. To see how well your symptoms are under control, your healthcare provider may ask you to keep a symptom diary at home, either on paper or in an app (for example: MaskAir app). This helps your doctor adjust your treatment so you can get the most benefit from your therapy.

Washing out the nose with saline after allergen exposure also helps. Nasal rinsing with saline (salt water) is an effective, low-risk, inexpensive, non-pharmacological treatment option for managing allergic rhinitis symptoms in adults and children. Nasal rinsing can:
Using a rinse 15 minutes before applying other medications to your nose (like corticosteroid sprays) can also help those medicines work better by allowing them to reach the inside of your nose more effectively.
Nasal rinsing with saline has few side effects, except that you need to learn how to do it properly to avoid discomfort. Nasal rinsing can be safely done every day.
You can learn how to make your own saline solution, explore the different rinsing devices available, and follow step by step instructions for using each type of device. We’ve also created a helpful video with tips and tricks on how to care for and maintain your nasal rinsing equipment.
It is important to use clean water. In some countries, it is safe to use tap water.
However, always follow your healthcare provider’s instructions and, in case of doubt, use commercially bottled still water, distilled water, or previously boiled and cooled down tap water to prepare the saline solution.
You can download your own copy of our nasal rinsing leaflet to keep nearby when performing rinses at home. It will guide you through the process and help you get the most out of this treatment.
(examples: mometasone, fluticasone, ciclesonide)
Nasal corticosteroid sprays are an effective, and first-line treatment option for easing the nasal and eye symptoms caused by allergic rhinitis. They reduce nasal congestion and are considered the preferred option for long term symptom control. Studies have shown that nasal corticosteroid sprays are more effective than oral antihistamines for symptom relief, and they provide relief of symptoms for a lot of people. Some nasal corticosteroid sprays are available over-the-counter, while others require a prescription.
Nasal corticosteroid sprays:
• Reduce inflammation inside your nose
• Reduce stuffiness, runny nose, itching and sneezing over time
• Reduce eye symptoms that are often associated with allergic rhinitis
Consistent use is important, as these sprays do not provide immediate relief. It can take up to two weeks for the nasal spray to work fully. If your symptoms are very strong at the beginning, you may need an additional medicine, such as a nasal antihistamine, for a short time until the nasal corticosteroid reaches its full effect.
Maximal effect is achieved with daily use. If you find it difficult to remember your nasal spray, try keeping it next to your toothbrush or linking it to another daily routine so you don’t forget.
Because of how these medicines work, they are not very helpful for one off or occasional allergen exposure. For example, if you’re allergic to animal dander, this type of treatment won’t give quick relief when visiting someone who has pets. Antihistamines would be more appropriate in this case.
Corticosteroid sprays are safe to use in the long term. Some people can experience side effects like irritation, nose bleeding or nasal dryness. However, a correct spraying technique can prevent most of the discomfort.
Learn how to use your nasal spray the right way. This helps it work better and reduces the chance of side effects. Some 70 % of AR sufferers referred to a tertiary centre were satisfied with their nasal corticosteroid treatment once that had been shown how to use it correctly and did so regularly in the long term.
The different types of sprays differ with regard to the frequency of doses, the spray device used, and the cost, but all are similarly effective for treating all of the symptoms of allergic rhinitis.
It is best to use those that need once daily application with least corticosteroid absorption i.e.: fluticasone propionate and furoate, mometasone furoate and ciclesonide- especially in children, in long term use and in patients with asthma or eczema who may be using corticosteroid elsewhere.
(examples: azelastine, olopatadine)
Antihistamine nasal sprays can be used twice every day or only when you need them, such as during occasional exposure to allergens. They start working within minutes. While they help relieve symptoms like a runny nose, nasal itch, and sneezing, they are less effective at relieving nasal congestion. Nasal antihistamine sprays are more effective than antihistamine tablets, work within 15 minutes and very safe when used as directed. The most common side effect is an unpleasant taste, which can usually be avoided by using the correct nasal spray technique. Gargling some ten minutes after use can help.
(azelastine/fluticasone, olopatadine/mometasone,)
Nasal sprays that combine a corticosteroid with an antihistamine often relieve allergic‑rhinitis symptoms better than using either type of spray on its own. They are usually considered a second‑line treatment, meaning they are used when a single medicine does not provide enough symptom control. These combination sprays are more expensive and depending on where you live, you might need a prescription and because they contain both medicines, they can cause the same side effects that each treatment may cause individually. The spray starts working quickly, often within minutes, but it needs to be used regularly to reach its full effect. Taking it consistently helps keep your symptoms under better control. In some countries these are available over the counter at the pharmacy.
(examples: oxymetazoline, xylometazoline)
Nasal decongestants are the most powerful nasal treatment for nasal congestion. They squeeze shut the nasal blood vessels and display a fast onset of action. They are often available over-the-counter. However, they are not recommended for the treatment of allergic rhinitis. The decongested nose becomes too open and does not function well as a mobile air purifier and humidifier and there is a risk of damage to the nose if the decongestant spray is used for more than a few days.
For allergies, it is better to use treatments that can be used safely for weeks or months, such as nasal corticosteroid sprays.
If a nasal decongestant spray is used to provide short term relief from severe congestion, it should be limited to a maximum of 7 days, and preferably less. A short course of nasal decongestant spray can be helpful during the first few days of starting a corticosteroid spray, while the corticosteroid is still building up to its full effect. However, decongestants should be stopped within 7 days. Using them longer can cause “rebound congestion,” meaning the spray itself starts causing nasal blockage when used for too long. This condition is called “rhinitis medicamentosa”. It means the nose stays blocked unless the decongestant spray is used again and again. Once this dependence develops, it can be difficult to break, which is why it’s so important to prevent it in the first place.
Cromolyn nasal spray helps prevent or reduce symptoms of allergic rhinitis, such as sneezing, a runny nose, and nasal itching. It works by targeting certain immune cells and preventing them from releasing the substances that trigger allergic reactions.
For cromolyn to work well, it needs to be used every day, several times a day. It can take several weeks to reach its full effect. Because of this delay, it’s recommended to start the treatment 1–2 weeks before allergy season begins, or be aware that it will take time to work if used for year‑round allergies. Cromolyn is not helpful for occasional exposures, such as briefly visiting a home with a pet. It is considered a very safe treatment, with only minor side effects reported, like sneezing or mild nasal irritation.
Ipratropium bromide nasal spray is used to treat the very runny nose. It does not help with other symptoms such as nasal congestion or sneezing. It works by reducing the activity of the nerves controlling fluid production and is mainly used in non-allergic rhinitis. Possible side effects include dryness of the nose, mouth, or throat, as well as mild nasal irritation. Its effect usually begins within 15 minutes, but it may take longer use to reach the best results.

(examples: loratadine, levocetirizine, fexofenadine)
Oral antihistamines are common, over-the-counter and prescription medications that help treat allergy symptoms. Antihistamines block the action of histamine, a chemical your body releases during an allergic reaction. By preventing histamine from attaching to its receptors, they help stop symptoms like sneezing, itching, and a runny nose.
Nasal antihistamine sprays can start working within minutes, while oral antihistamines may take a few hours to have their full effect. This means they can be taken on-demand (as needed) for symptom relief, but consistent daily dosing is typically needed for more persistent allergies. Oral antihistamines are less effective on nasal symptoms compared to nasal antihistamines.
Your personal preference, symptom pattern, and the cost of the medication all play a role in choosing what works best for you. When choosing an antihistamine, nonsedating options are necessary. Older antihistamines can cause drowsiness, which may affect activities such as driving or operating machinery. Newer, nonsedating antihistamines are designed to avoid this problem. Get help from your pharmacist or doctor to help select the appropriate antihistamine for your allergy treatment.
(examples montelukast, zafirlukast)
Leukotriene modifiers, also called leukotriene receptor antagonists (LTRAs), are oral medications that block leukotrienes, chemicals which cause allergy symptoms. They are weakly effective in most users and are generally employed as an add-on therapy for people that have both asthma and allergic rhinitis or in those who cannot tolerate nasal sprays. LTRAs are only available with a prescription. People generally have good tolerance of these medicines, but described side effects include mental changes (anxiety, irritability, nightmares, depression, aggression, thoughts of self-injury), flu-like symptoms and abdominal pain. Side effects are more common in children. Anyone on LTRAs should be carefully monitored.
(example pseudoephedrine)
Oral decongestants ease nasal blockage caused by allergic rhinitis. They work by contracting the blood vessels in the nose, which opens the nasal passages and makes breathing easier. Because they travel through the bloodstream, they can also affect blood vessels in other parts of the body, not just the nose. Therefore, these medicines should be used with caution by people with high blood pressure, heart rhythm problems, or an enlarged prostate. Your healthcare provider can help determine whether they are safe for you. Common side effects include trouble sleeping, loss of appetite, and a fast or pounding heartbeat.
EUFOREA does not recommend their use since nasal decongestants work better with fewer side effects.
(examples methylprednisolone – prednisolone)
Steroids are medicines that help reduce inflammation. Oral steroids – which are taken by mouth – should be used only for very severe symptoms of allergic rhinitis (such as very severe nasal congestion), and only when other treatments have not provided enough relief. They are not meant for routine or long term use as this can cause more harm than benefit. During a short course of oral steroids, you might experience side effects such as increased appetite, difficulty sleeping, or mood changes like irritability or anxiety. When taken regularly or over a longer period of time, oral steroids can also lead to other side effects, including osteoporosis, hypertension and/or diabetes.
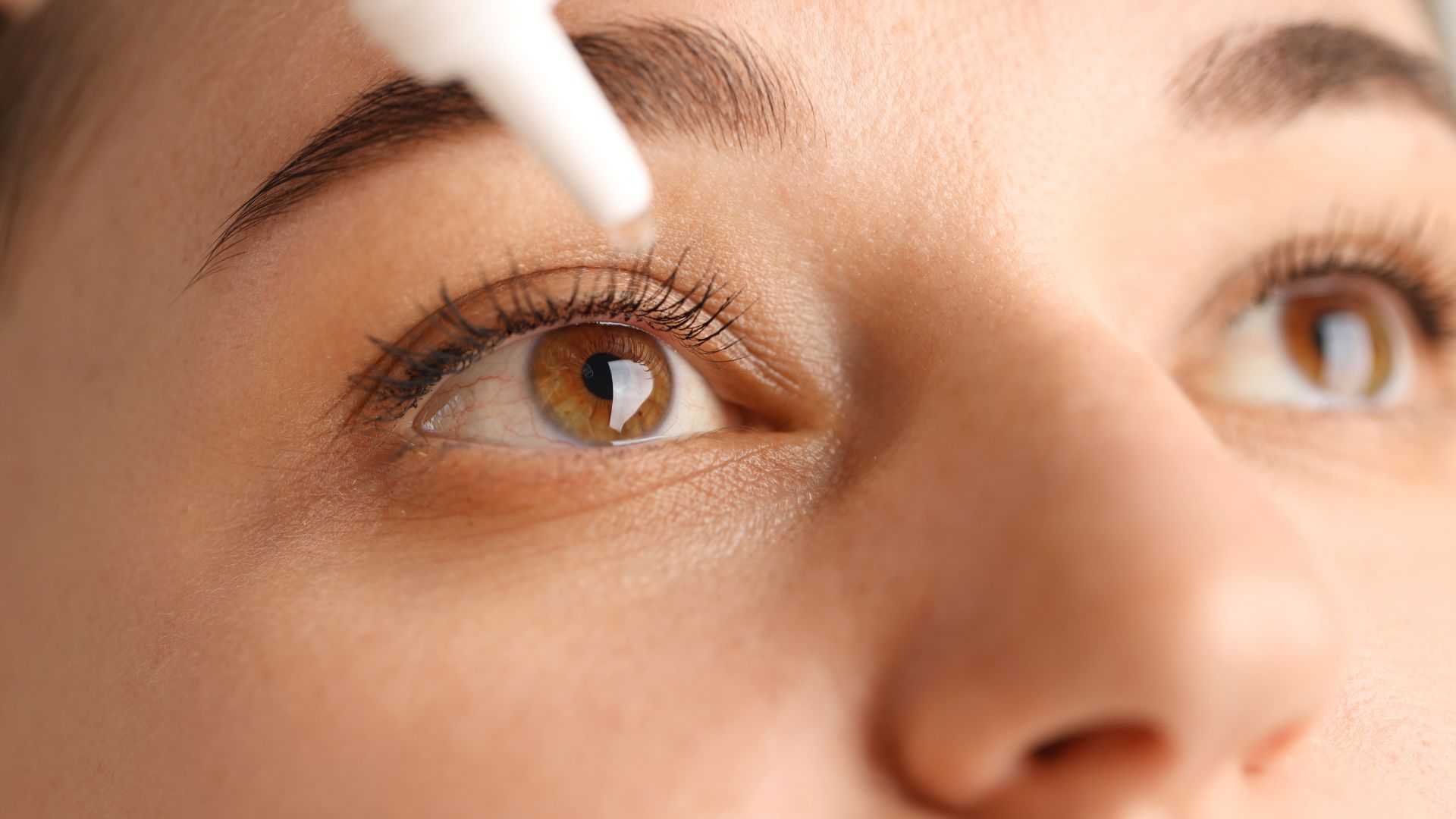
(examples: olopatadine, levocabastine)
Antihistamine eye drops help relieve itchy, red, watery eyes. Some eye drops are available over-the-counter, while others might require a prescription. They work rapidly, within minutes and are considered as a first-line treatment option for allergic conjunctivitis. Side effects are uncommon, but may include headache or dry eyes.
Cromolyn/nedocromil eye drops work by targeting certain immune cells and preventing them from releasing the substances that trigger allergic reactions. It helps prevent and treat symptoms of allergic conjunctivitis, including itchy, watery, red eyes. The main drawback is that it takes several days or up to a few weeks, to reach full effectiveness, so consistent daily use is essential. This makes this type of treatment unsuitable for as needed use. In addition, it requires frequent application throughout the day (4–6 times daily).
These eye drops are reserved for very severe eye disease and should only be prescribed and closely monitored by an eye specialist able to use slit lamp examination.
Learn how to use your eye drops the right way, as this can increase how effective they are while limiting side effects at the same time.

Allergen specific immunotherapy (AIT) is a treatment that helps guide the immune system away from an allergic response and toward developing tolerance. In other words, it works by gradually training the immune system to react less strongly to specific allergens over time. Research has shown that AIT can reduce the risk of developing new allergies, lower the chances of developing asthma, and provide long-lasting improvement in allergy symptoms even years after completing treatment.
AIT is usually continued for 3 to 5 years. Completing the full course is important to achieve long term benefits, even after treatment has stopped. Although it is not possible to predict exactly how long the effect will last for each individual, we know that the improvement generally persists for at least 2-3 years after stopping therapy.
AIT is available in two forms:
• Sublingual immunotherapy (SLIT): taken as tablets or drops under the tongue.
• Subcutaneous immunotherapy (SCIT): given as injections under the skin.
To find out whether allergen immunotherapy is a good option for you, an allergy specialist will perform formal allergy testing. This may include a skin prick test and/or a blood test to confirm which allergens are triggering your allergic rhinitis symptoms. AIT is usually reserved for people who continue to have symptoms despite using standard treatments for allergic rhinitis, or for those who are looking for a therapy that can offer longer lasting results.
With subcutaneous immunotherapy (SCIT), treatment starts with weekly injections in the hospital, using gradually increasing doses. After this initial phase, you move to the maintenance phase, where injections are given once a month. SCIT is associated with a small risk of a severe allergic reaction. This is why you are requested to stay in the waiting room for at least 30 minutes after every injection, so that you can receive immediate medical care if needed.
Sublingual immunotherapy (SLIT) has the advantage that it can be taken at home once the first dose has been monitored in the clinic. However, it requires commitment, as it must be taken daily for several years to achieve the best results. It is the safer form of allergen immunotherapy, with side effects usually limited to mild, local reactions in the mouth or throat, sometimes severe enough to cause people to stop the treatment. It may also be a more appealing option for people who dislike injections
Both SCIT and SLIT are only available for a limited number of allergens. It is very important to use a well – validated product which contains the allergen to which you react.
Learn more about all the practical aspects of AIT in the video below:
Nasal surgery is not a treatment for allergic rhinitis per se. However it may be necessary if the nasal structure prevents the proper use of therapeutic nasal sprays, for example if the nasal septum (the thin wall that divides the nasal cavity into two halves) is badly deviated. Whether surgery is appropriate will always be part of a thorough discussion with your ENT specialist, who will determine if it can play a role in your individual treatment plan.
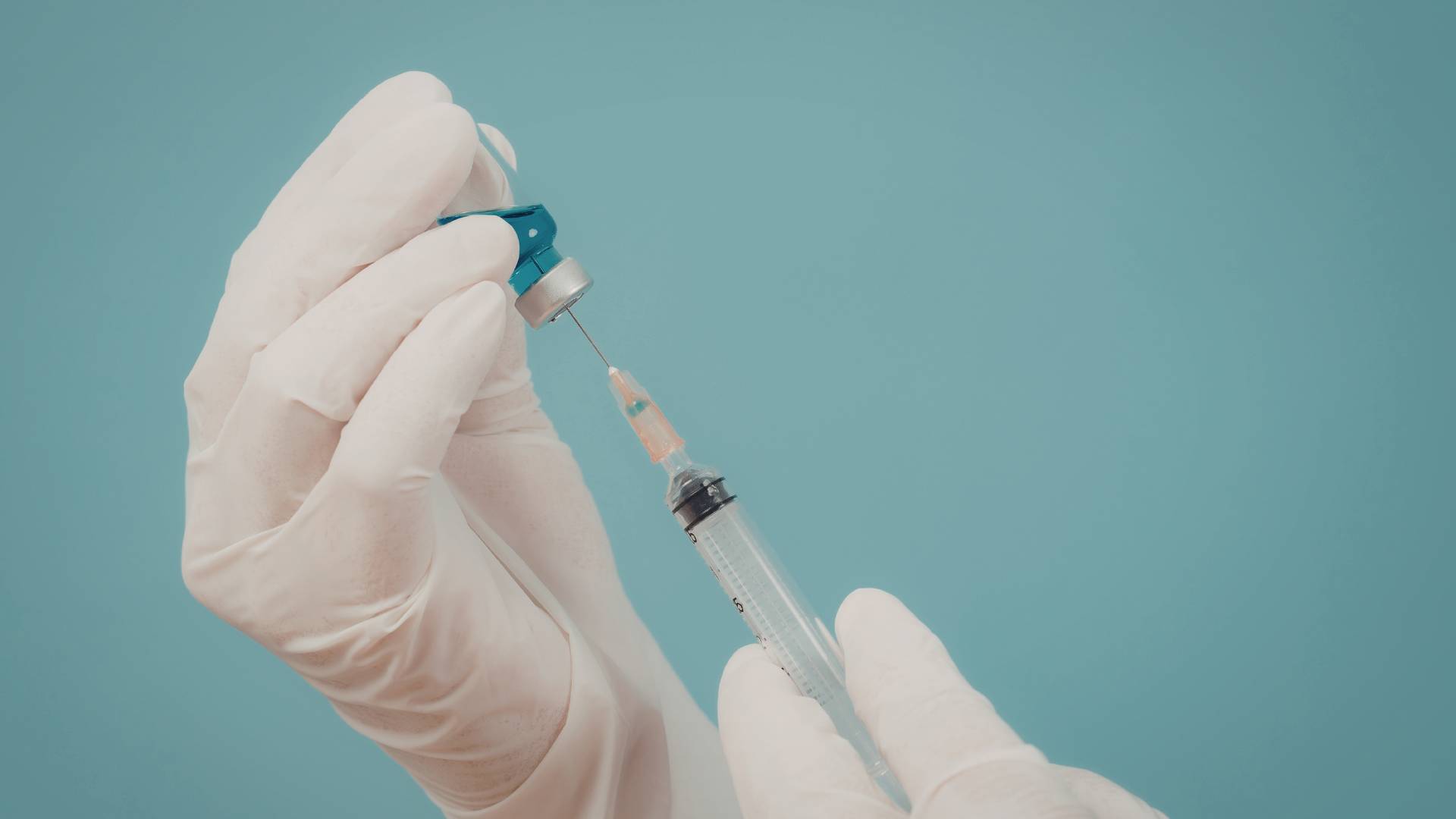
Depot corticosteroid injections should NOT be used for allergic rhinitis. Even though they are still sometimes offered, they carry a risk of serious side effects and are strongly discouraged by clinical guidelines. Your doctor will help you choose safer and more effective treatment options that are recommended for managing allergic rhinitis.
Although it can be tempting to look for other ways to manage your nasal or eye symptoms, there is very limited high-quality scientific research to support the use of complementary and alternative therapies in people with allergic rhinitis. That is also why their use is not proposed in international guidelines on the treatment of allergic rhinitis. It is also important to realize that in many countries, herbal medicines are minimally regulated and not often tracked in terms of side effects. If you’re thinking about trying any alternative or complementary treatments, always talk to your healthcare provider first to make sure they are safe and suitable for you.

Of course pregnant and breastfeeding women can also suffer from allergic rhinitis. During this important time during a woman’s life, treatment needs to be safe for both the mother and the child. Nasal saline rinsing is a safe non-medical option to be used throughout pregnancy and breastfeeding. When medication is needed to suppress symptoms, local treatment is preferred in case of local symptoms (eye drops, nasal sprays) because absorption into the bloodstream is low, making harm to the unborn child less likely. Although it is considered low-risk, it should only be used when clearly needed. Cromolyn nasal spray or eye drops are generally considered safe for use during pregnancy. Ocular antihistamines can also be used. By using the right eye drop technique, absorption in the blood stream can be limited even more.
If nasal corticosteroid sprays are necessary to adequately control symptoms, preference should be given to those sprays with low absorption into the bloodstream, such as fluticasone. The use of oral antihistamines in pregnant women has been studied and the non-sedating antihistamines (levo)cetirizine and (des)loratadine are the preferred options during pregnancy. Decongestants, nasal antihistamines, and leukotriene modifiers should be avoided during pregnancy.
During breastfeeding, local treatments (eye drops/nasal sprays) remain the preferred option. They only contain small doses of medication and the chances of those reaching the baby via the breastmilk are very slim. If you need to take antihistamines during breastfeeding, cetirizine and loratadine are one of the best options. Small occasional doses of these medications are acceptable during breastfeeding. Larger doses or more prolonged use may cause drowsiness and other effects in the newborn or decrease the mother’s milk supply.
This website does not provide medical advice.
The information, including but not limited to, text, graphics, images, and other material contained on this website is for informational purposes only. No material on this site is intended to be a substitute for professional medical advice, diagnosis, or treatment and/or medical treatment of a qualified physician or healthcare provider. EUFOREA is not a medical organisation and cannot provide specific medical advice to patients via the Internet and/or E-mail. All patients are encouraged to direct their specific questions to their personal physicians. EUFOREA presents this information to patients so that patients can understand and participate in their own medical care. EUFOREA strongly emphasises that the information contained on this website is not a substitute for thorough evaluation and treatment by a qualified healthcare provider.
© 2025 - EUFOREA - All rights reserved. All content on this portal, such as text, graphics, logos and images, is the property of EUFOREA. They may not be reproduced, copied, published, stored, modified or used in any form, online or offline, without prior written permission of EUFOREA.